 During the mid-1800s, there were two major theories on the cause of cholera being debated widely in medical circles throughout London. The organism that caused cholera, Vibrio cholerae, was not yet known and would not be until 1883, twenty-five years after the death of John Snow. In that year, Robert Koch, a German physician and bacteriologist, discovered the etiologic microbe. [SOURCE]
During the mid-1800s, there were two major theories on the cause of cholera being debated widely in medical circles throughout London. The organism that caused cholera, Vibrio cholerae, was not yet known and would not be until 1883, twenty-five years after the death of John Snow. In that year, Robert Koch, a German physician and bacteriologist, discovered the etiologic microbe. [SOURCE]
MIASMA THEORY
Many in the early to mid-nineteenth century felt that cholera was caused by bad air, arising from decayed organic matter or miasmata. “Miasma” was believed to pass from cases to susceptibles in diseases considered contagious. Believers in the miasma theory stressed eradication of disease through the preventive approach of cleansing and scouring, rather than through the purer scientific approach of microbiology. One prominent supporter of the miasma theory was Dr. William Farr, then assistant commissioner for the 1851 census and a career employee of the government’s General Register Office. For a while, Farr was convinced that cholera was transmitted by air. He reasoned that soil at low elevations, especially near the banks of the River Thames, contained much organic matter which produces miasmata. The concentration of such deadly miasmata would be greater at lower elevations than in communities in the surrounding hills. His calculations in 1852 seemed to support this theory (see chart below for a 1961 redrawing of Farr’s 1852 calculations).
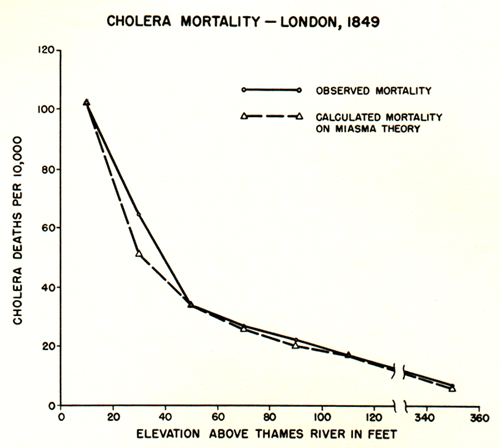
Source: Graph illustrating Farr’s elevation theory in Langmuir AD. Bacteriological Review 25, 174, 1961.
GERM THEORY
The alternative theory, supported by John Snow, held that cholera was caused by a germ cell, not yet identified. He reasoned that this germ was transmitted from one person to another by drinking water. Snow’s germ theory was deemed “peculiar” by John Simon, head medical officer of London, but has since met the test of time. What was this peculiar theory?
Here is a summary written by Dr. Simon:
“This doctrine is, that cholera propagates itself by a ‘morbid matter’ which, passing from one patient in his evacuations, is accidentally swallowed by other persons as a pollution of food or water; that an increase of the swallowed germ of the disease takes place in the interior of the stomach and bowels, giving rise to the essential actions of cholera, as at first a local derangement; and that ‘the morbid matter of cholera having the property of reproducing its own kind must necessarily have some sort of structure, most likely that of a cell.”
While Dr. Simon clearly understood John Snow’s theory, he joined others in questioning the relevance of the germ theory to cholera.
WILLIAM FARR
For some while, William Farr was the leader of the “pro-miasma” health scientists. Yet later, he changed his mind as Snow’s data were published, and other supporting facts appeared. So who was William Farr? As it turns out, his origin was very similar to John Snow’s, coming from a lower socio-economic class background.
 Farr, William (1807-83), like John Snow, was the child of a farm laborer. He was born on November 30, 1807 at Kenley in Shropshire. Fortunately, at an early age he was adopted or at least financially supported by Joseph Pryce of Shrewsbury, the squire of his parents’ community. His early years were spent studying at public day schools, supplemented with tutoring by a local minister.
Farr, William (1807-83), like John Snow, was the child of a farm laborer. He was born on November 30, 1807 at Kenley in Shropshire. Fortunately, at an early age he was adopted or at least financially supported by Joseph Pryce of Shrewsbury, the squire of his parents’ community. His early years were spent studying at public day schools, supplemented with tutoring by a local minister.
Age 19. In May 1826, he joined the staff of a local infirmary in Shrewsbury, commuting from home six days a week for the next two years. His preceptor was Dr. Webster.
Age 21. His early benefactor, Joseph Pryce, died in November 1828 and left William Farr a small inheritance. The money was enough to take Farr to Paris, France a few months later to study medicine. Farr remained in Paris from April 1829 to July 1830, when the July Days insurrection overtook France.
Age 23-25. On returning to England, Farr attended medical lectures at University College, London from 1830-32. In March 1832, he passed the examination of the Society of Apothecaries which allowed him to practice medicine. Early the next year, he married and both lived and had his medical practice at 8 Grafton Street in Fitzroy Square.
Age 28. Rather than continuing with his private practice, Farr turned increasingly to medical journalism. At first he wrote articles that appeared in The Lancet. Beginning in 1835, he served as a medical editor of the British Medical Almanack and then started editing his own journal.
Age 30. Farr’s wife died of tuberculosis in 1837, which stimulated a life-long interest in this disease. In the same year, his medical preceptor, Dr. Watson, also died and left him both money and his library.
Age 31. In 1838, Farr obtained the post of compiler of abstracts (i.e., birth and death certificates) in the registrar general’s office. He remained with this government agency for forty years, rising eventually to superintendent of the Statistical Department.
Age 35. Farr married his second wife in 1842 and had eight children in the following years.
Over time he became well-known for his use of vital statistics, and published much of his work in Reports of the Registrar-General, 1839-80, the same publication used by John Snow to test the germ theory of cholera.
Age 47. In 1854, Farr was appointed member of the Scientific Committee for Scientific Enquiries in Relation to the Cholera Epidemic of 1854. Given his support of the miasma theory, this platform lead to conflicts with John Snow. A report was issued in 1855.
Farr’s Committee wrote:
“In explanation of the remarkable intensity of this outbreak [Broad Street Pump outbreak] within very definite limits, it has been suggested by Dr. Snow, that the real cause of whatever was peculiar in the case lay in the use of one particular well, situated at Broad Street in the middle of the district, and having (it was imagined) its waters contaminated with the rice-water evacuations of cholera patients. After careful inquiry, we see no reason to adopt this belief. We do not feel it established that the water was contaminated in the manner alleged; nor is there before us any sufficient evidence to show whether inhabitants of that district, drinking from that well, suffered in proportion more than other inhabitants of the district who drank from other sources.”
The Committee added support to the miasma theory when elsewhere in the 1855 report they concluded:
“But, on the whole of evidence, it seems impossible to doubt that the influences, which determine in mass the geographical distribution of cholera in London, belong less to the water than to the air.”
Age 59. By 1866, eight years after the death of John Snow, medical opinion had changed to support the germ theory of cholera and its waterborne transmission. Farr wrote a detailed report in 1866 that relied heavily on his extensive knowledge of statistics. Using death rates to justify his conclusions, he publicly acknowledged that water was the most important means of transmission, not miasmata as previously stated.
Age 75. Shortly after his retirement, William Farr died due to bronchitis on April 14, 1883, the same year Robert Koch discovered Vibrio cholerae. Three years earlier in 1880, he had received the Gold Metal of the British Medical Association, acknowledging his considerable contributions to the field of biostatistics. Farr had outlived John Snow by 25 years, but long since recognized the error of the miasma theory as the cause of cholera transmission.
Debate and Legislative Action
The debate between supporters of the miasma and germ theories extended well beyond cholera and had major legislative impact. The debate also invoked a strong editorial in The Lancet, highly critical of John Snow for his germ theory views. To read more, click here.
Search for Patterns
John Snow spent most of Tuesday searching for patterns. He knocked on doors, talked to strangers in the street, trying to find any anecdotal evidence about the outbreak and its victims. He stopped at the Register-General’s Office, where Farr gave him the numbers that had been calculated for the week. Eighty-three deaths had been reported in Soho between Thursday and Saturday. Snow stopped at the Broad Street Pump and reviewed the addresses of the dead. He knew he was going to need more than addresses to prove the pump was the culprit. He would need footprints too.
Next: Building a Case and The Pump Handle
Sources:
Eyler JM. Victorian Social Medicine — the Ideals and Methods of William Farr, 1979.
Last J (ed). A Dictionary of Epidemiology, 1995.
Paneth N, et al. American J Public Health 88, 1545-53, 1998.
Pelling M. Cholera, Fever and English Medicine, 1825-65, 1978.
Stephen L and Lee S (eds). Dictionary of National Biography, Vol. 6, Oxford University Press, 1921-2.
Wohl AS. Endangered Lives — Public Health in Victorian Britain, 1983.